Reversing Cervical Spinal Fusion with Dr. Alexander Taghva
Dr. Alexander Taghva is a board-certified neurosurgeon in Orange County who specializes in motion-preserving spine surgery including artificial disc replacement and cervical fusion reversal procedures. Artificial cervical disc procedures allow selected patients to achieve neck motion restoration through the removal of their previous fusion. The procedure requires technical expertise as multiple factors must be assessed to determine who qualifies for it.

Can a Cervical Spinal Fusion Be Reversed?
Yes. In certain cases, a cervical fusion can be taken out and converted to an artificial disc replacement. I’m getting asked this question more and more in my practice, and the short answer is that it’s possible — but there are strict criteria that have to be met.
Why Would You Want to Reverse a Fusion?
I think about it in two ways.
The first is motion preservation. A fusion eliminates movement at the treated segment. You lose some range of motion in your neck, primarily in flexion and extension. (Rotation is mostly handled higher up at C1-2, so that’s less affected.) Reversing the fusion and replacing it with an artificial disc can restore that lost motion.
The second reason — and I think this is actually the bigger deal — is preventing adjacent segment disease. When one level of the cervical spine is fused, the levels above and below have to pick up the slack. Over time, that extra stress can accelerate degeneration at those neighboring segments, sometimes leading to new herniations, stenosis, and the need for additional surgery. Converting a fusion to a disc replacement removes that mechanical stress and may protect those adjacent levels long-term.
Are you ready to meet a leading Orange County Neurosurgeon?
Who is a Candidate?
Not everyone with a cervical fusion can have it reversed. The criteria are specific:
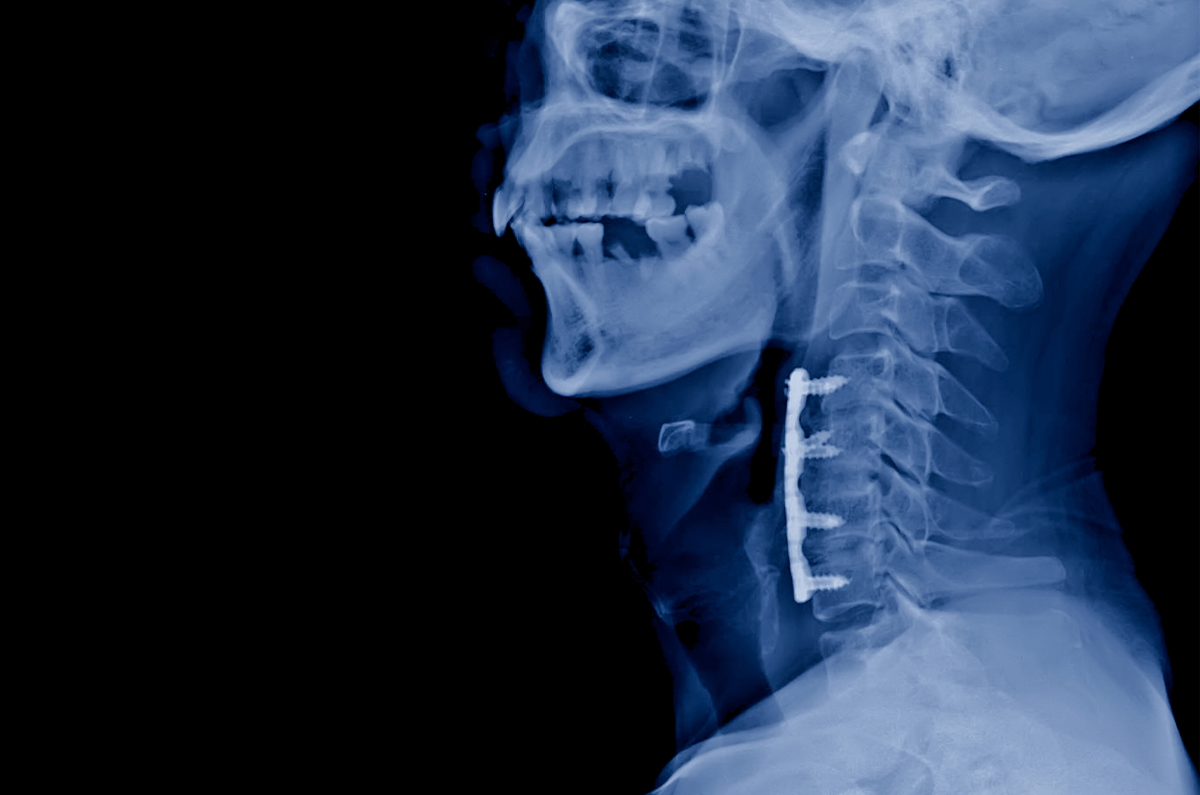
The original surgery must have been an anterior-only approach. That means an anterior cervical discectomy and fusion (ACDF). If the back of the spine was involved — particularly the facet joints — we don’t have a good way to replace that motion. So this only applies to patients whose surgery was done from the front of the neck.
The original reason for surgery should be degenerative disc disease or a herniated disc — not trauma. In the setting of a fracture, even if the bone heals, we often don’t know the condition of the muscles and ligaments surrounding the spine. If we undo the fusion and put in an artificial disc, those soft tissue structures may not be able to provide the stability the disc needs. Degenerative cases are more predictable.
The facet joints can’t have fused on their own. This sometimes happens even when only an anterior fusion was performed. The posterior joints gradually ankylose over time and lose their ability to move. Every candidate for fusion reversal needs a full workup: X-rays, a CT scan of the cervical spine, and an MRI. The CT in particular tells me whether the facets have auto-fused.
More recent fusions tend to be better candidates. This is a softer criterion, but I’ve found it matters. Patients who had their fusion done more recently tend to have less bony integration into the cage and hardware, which makes the implant easier to remove. There’s also a practical reality: if a motion segment has been locked in place for years, it takes longer for the body to readjust to having motion there again, and longer to rebuild range of motion through that segment. A fusion done one or two years ago is generally a more straightforward conversion than one done ten years ago.
What the Surgery Involves
This is not a simple procedure. Converting a fusion to an artificial disc involves removing the existing hardware and bone graft, clearing scar tissue, making sure there’s no residual compression of the nerves or spinal cord, and then placing an artificial disc into the prepared space. It’s technically demanding, and the anatomy is different from a primary operation because of the scar tissue and altered bone structure from the original surgery.
There are also situations where the imaging looks favorable but we encounter something unexpected during the operation — instability we didn’t anticipate, or bone quality that can’t support an artificial disc. It doesn’t happen often, but it’s a real possibility, and every patient considering this needs to understand that going in.
Insurance and Cost
Right now, conversion of a fusion to an artificial disc is not covered by insurance. This is an out-of-pocket procedure. The cost includes operating room time, anesthesia, intraoperative neuromonitoring (which I use for all of these cases), the artificial disc implant itself, surgical equipment, and the surgeon’s fee. I’ll give you a full financial picture during your consultation so there are no surprises.
Is This Procedure Right for You?
If you’ve had an ACDF and you’re dealing with stiffness, lost range of motion, or early signs of adjacent segment degeneration, it’s worth a conversation. I’ll explain to you in direct terms which cases of your condition can be treated with reversal. The imaging tells most of the story; bring your CT and MRI to the consultation, and we’ll go through it together.

Why Choose Dr. Alexander Taghva
Dr. Alexander Taghva is a leading board-certified neurosurgeon, specializing in brain surgery, endoscopic spine surgery, as well as spine disorders. Also, he is the only spine surgeon in Orange County and southern California who offers endoscopic laminotomy surgery. Dr. Taghva:
- Graduated from Johns Hopkins University School of Medicine and completed his residency at the University of California
- Completed a prestigious fellowship at The Ohio State University in Neuromodulation and Functional Neurosurgery
- Specializes in minimally invasive and endoscopic surgery, spinal stenosis, artificial disc replacement, spinal disorders, spinal surgery revision, and other spinal conditions.
- Specializes in brain surgery to treat trigeminal neuralgia, brain tumors, pituitary tumors, and Parkinson’s disease.
- A highly-respected neurosurgeon with many years of experience, including treating chronic pain via stimulation of the spinal cord and brain
- Actively involved in medical research and the lead investigator for clinical trials on spinal cord stimulation




