Spinal Cord Stimulation Orange County, CA with Dr. Taghva
Spinal cord stimulation is an implantable device that delivers mild electrical pulses to the spinal cord, interrupting pain signals before they reach the brain. It doesn’t fix the structural problem that caused the pain, but it changes how the nervous system processes it. For the right patient, that distinction is the difference between being on disability and going back to work.
I implant spinal cord stimulators for patients with chronic pain that hasn’t responded to other treatments. Most commonly I treat failed back surgery syndrome, complex regional pain syndrome (CRPS), and persistent leg pain, arm pain, back pain, or neck pain after spine surgery. These are patients who’ve been through the cycle: physical therapy, injections, maybe one or two surgeries, and they’re still hurting. SCS gives them an option that doesn’t involve another structural operation.

Why I think about SCS differently than most spine surgeons
Most spine surgeons are trained to operate on anatomy. Decompress a nerve, fuse a segment, replace a disc. When that doesn’t work, they don’t always have a next move. I do, because I trained specifically in neuromodulation, which means my toolkit doesn’t end when the structural surgery options run out.
That matters because the patients who benefit most from spinal cord stimulation are often the ones other surgeons have given up on. They’ve been told their MRI looks fine, or that there’s nothing left to do, or that they should just manage the pain with medication. SCS works on a different axis entirely. It targets the electrical signaling of pain itself, not the mechanical structure of the spine.
I was one of the first surgeons in Southern California to implant the Nevro Senza high-frequency stimulator, and I was the first in Orange County to perform endoscopic spinal cord stimulator placement. I work with devices from all the major manufacturers — Abbott, Boston Scientific, Medtronic, Saluda, and Nevro — because the technology is evolving fast and no single device is best for every patient.
How spinal cord stimulation works
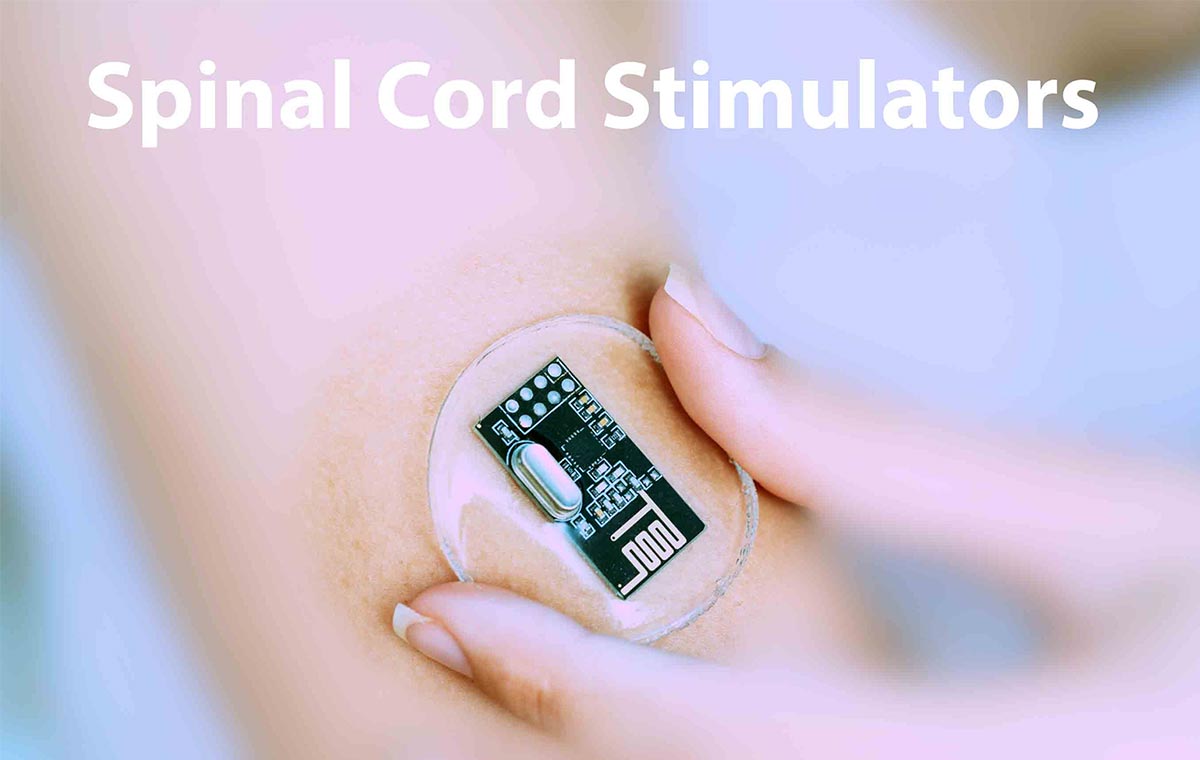
A thin wire with electrical contacts (the lead) is placed in the epidural space of the spine, near the spinal cord. The lead connects to a small battery-powered generator implanted under the skin, usually in the upper buttock or lower abdomen. The device delivers electrical pulses that modulate pain signaling . Some systems produce a mild tingling sensation, others work below the level of perception so you don’t feel anything at all.
The key concept is that the stimulation can be adjusted. If your pain changes, the programming changes with it. If you don’t like it, the device can be turned off or removed entirely. That reversibility is one of the strongest arguments for SCS. And unlike a fusion or another structural surgery, you’re not burning any bridges.
Are you ready to meet a leading Orange County Neurosurgeon?
The trial period
Before committing to a permanent implant, every patient undergoes a trial. I place temporary leads through a needle and you wear an external generator for about a week. You go home, live your life, and see how much relief you get. If the trial reduces your pain by at least 50%, we proceed with the permanent implant. If it doesn’t, we remove the leads in the office and you’ve lost nothing but a week.
This trial-first approach is one of the things I like most about SCS. It’s the only major pain intervention where you get to test-drive the result before committing to it.
What the permanent implant involves
The permanent procedure takes about an hour and is done under general anesthesia. I place the leads either percutaneously (through a needle) or using a small open approach to position a paddle lead directly over the spinal cord. Paddle leads provide more precise stimulation coverage and tend to use less battery, but they require a small laminotomy incision. The choice depends on where your pain is and what the trial told us about optimal lead position.
The generator is implanted under the skin through a separate small incision. Most patients go home the same day. Recovery is straightforward — you’ll limit bending and twisting for a few weeks while the leads settle into position, then gradually return to normal activity.
Who is a candidate
SCS works best for neuropathic pain — pain that comes from damaged or dysfunctional nerves rather than an ongoing structural problem. Good candidates typically have:
- Chronic leg pain, arm pain, back pain or neck pain after previous spine surgery (failed back surgery syndrome or persistent spinal pain syndrome)
- Complex regional pain syndrome (CRPS/RSD)
- Peripheral neuropathy with refractory pain
- Pain that isn’t well-explained by current imaging — meaning the MRI doesn’t show something that another surgery would fix
SCS is not a first-line treatment. It’s for patients who’ve exhausted conservative options and aren’t good candidates for further structural surgery. If I think a decompression or disc replacement would solve the problem, I’ll recommend that instead. SCS is the tool I reach for when the structural answers have been tried or don’t apply.

What SCS doesn’t do
It doesn’t cure the underlying condition. It doesn’t always eliminate pain completely — the goal is meaningful reduction, not perfection. And it requires some ongoing maintenance: programming adjustments, battery replacements (every 5–10 years for non-rechargeable units, 10+ years for rechargeable), and occasional follow-up imaging. I’m transparent about these realities because I think patients make better decisions when they have accurate expectations.

Why Choose Dr. Alexander Taghva
Dr. Alexander Taghva is a leading board-certified neurosurgeon, specializing in brain surgery, endoscopic spine surgery, as well as spine disorders. Also, he is the only spine surgeon in Orange County and southern California who offers endoscopic laminotomy surgery. Dr. Taghva:
- Graduated from Johns Hopkins University School of Medicine and completed his residency at the University of California
- Completed a prestigious fellowship at The Ohio State University in Neuromodulation and Functional Neurosurgery
- Specializes in minimally invasive and endoscopic surgery, spinal stenosis, artificial disc replacement, spinal disorders, spinal surgery revision, and other spinal conditions.
- Specializes in brain surgery to treat trigeminal neuralgia, brain tumors, pituitary tumors, and Parkinson’s disease.
- A highly-respected neurosurgeon with many years of experience, including treating chronic pain via stimulation of the spinal cord and brain
- Actively involved in medical research and the lead investigator for clinical trials on spinal cord stimulation




