Basivertebral Nerve Ablation for Chronic Low Back Pain
Not every back pain is a disc. Not every back pain is a facet. And a lot of patients with persistent, deep, midline low back pain have been told their problem is “nonspecific” — which usually means nobody has figured out where the pain is actually coming from.
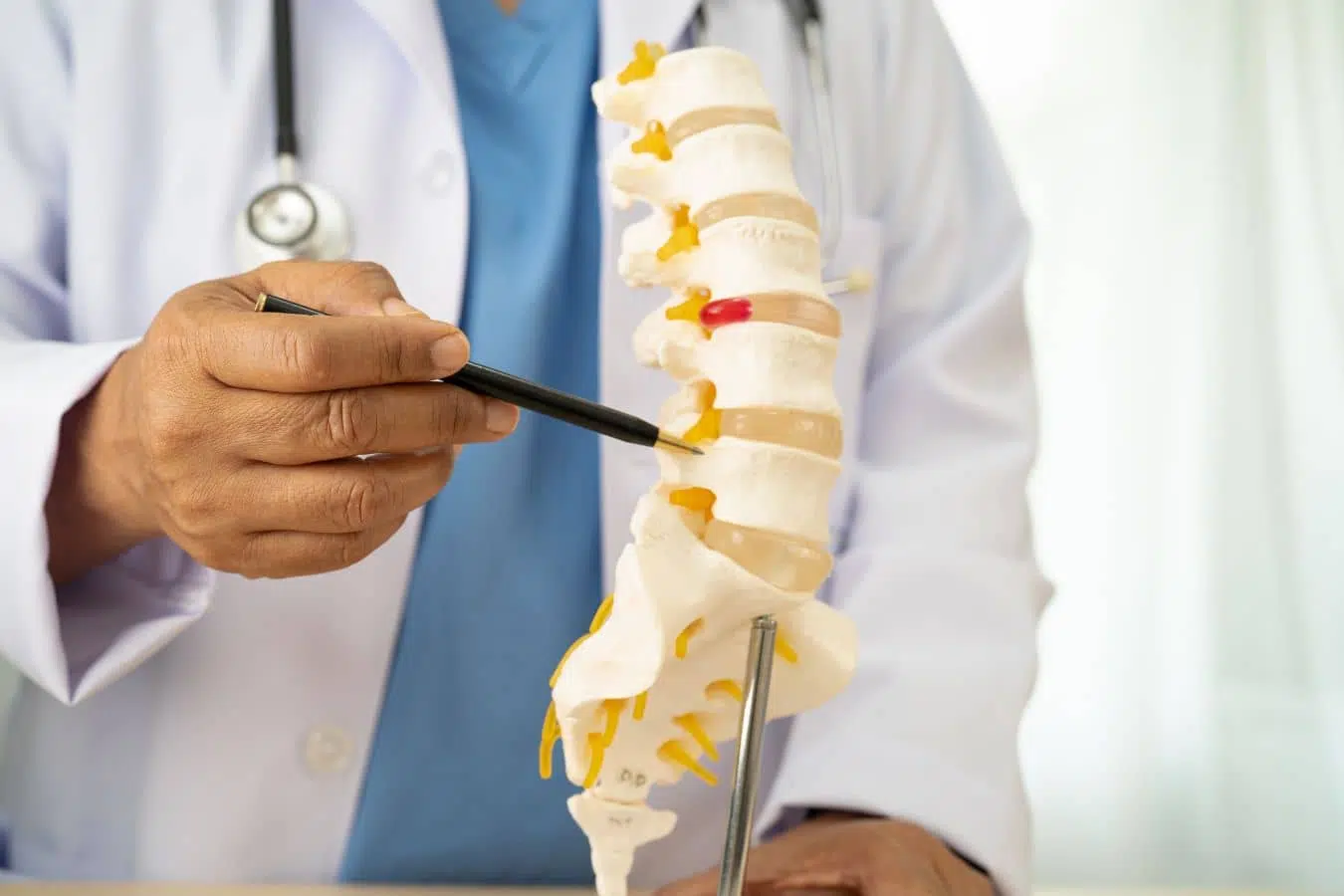
Basivertebral nerve ablation targets a pain generator that most spine surgeons don’t talk about: the vertebral body itself. Inside the hard shell of each vertebra, there’s a network of nerves called the basivertebral nerve complex. For a long time, we thought these nerves were just maintenance workers — trophic nerves responsible for regulating bone density. It turns out they can carry pain signals. When the protective endplate of the disc wears down, the bone underneath gets inflamed. That inflammation irritates the basivertebral nerve, sending a deep, hard-to-localize ache to the brain.

Patients describe it perfectly: “bone-deep” pain. It doesn’t follow the usual rules. It doesn’t clearly get worse with extension the way facet pain does. It doesn’t radiate into the leg the way a compressed nerve does. It just sits there in the low back, often worse with sitting and flexion, and it’s resistant to the standard treatments — because those treatments are aimed at the wrong target.
Why standard treatments miss it
This is a pain generator that lives inside bone. You can’t massage a bone. An epidural injection sits outside the bone. Physical therapy strengthens muscles around the spine but doesn’t address inflammation inside a vertebral body. Facet injections and nerve blocks target structures behind the spine, not inside it. This is why patients with vertebrogenic pain cycle through PT, injections, and frustration without getting better. The treatments aren’t failing — they’re aimed at the wrong address.

Call today to Schedule your Consultation
Dr. Alexander Taghva delivers advanced spine and brain solutions.
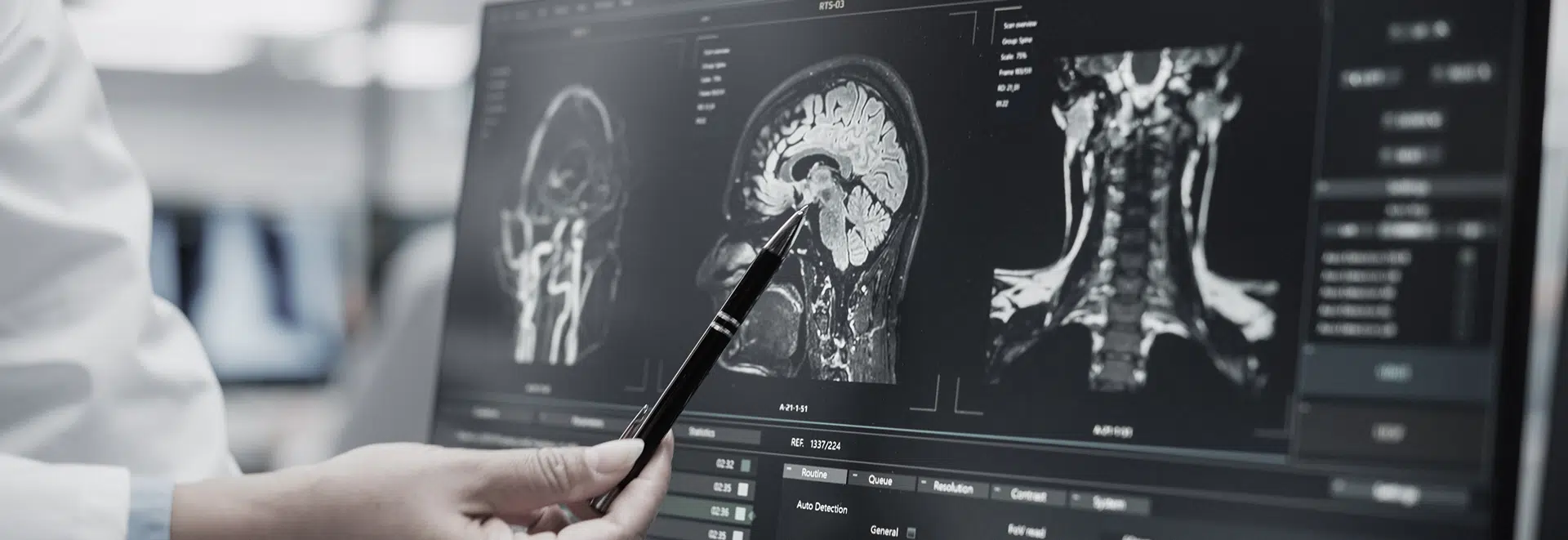
The MRI clue
The key diagnostic finding is something called Modic changes on MRI. These are signal changes within the vertebral body endplates that most radiologists report but many clinicians gloss over.
Type 1 Modic changes are the ones that matter most. The bone marrow looks bright on certain MRI sequences, representing active inflammation and edema inside the bone. This is the painful phase — the basivertebral nerve is being irritated by an inflammatory process in the marrow itself.
Type 2 Modic changes represent the burned-out phase, where the marrow has converted to fat and the acute inflammation has settled. These are generally less painful.
When I see a patient with deep, midline low back pain, no radiculopathy, no clear surgical target, and Type 1 Modic changes at one or two levels — that’s a pattern. It’s not “nonspecific low back pain.” It’s vertebrogenic pain, and it has a specific treatment.
How basivertebral nerve ablation works
The procedure is straightforward in concept. Under fluoroscopic (X-ray) guidance, a specialized probe is threaded through the pedicle of the vertebra into the vertebral body, navigating to the trunk of the basivertebral nerve near the midline of the bone. Radiofrequency energy is then delivered through the probe, heating the nerve and ablating it — permanently interrupting its ability to transmit pain signals.
It doesn’t fix the disc. It doesn’t fuse the bone. It doesn’t change the structure of the spine at all. What it does is cut the telephone line that’s sending the pain signal from the inflamed bone to the brain.
The procedure is performed as an outpatient surgery. Patients go home the same day. There’s no hardware left behind, no implant, no device to maintain. The ablation is a one-time procedure.
Who is a candidate
The candidacy criteria are specific, and that’s actually one of the strengths of this procedure — when the patient fits the pattern, the results are reliable.
Good candidates typically have:
- Chronic low back pain lasting at least 6 months
- Pain that is primarily midline and axial — centered in the low back, not radiating into the legs
- Pain that is worse with sitting and flexion loading
- No radiculopathy (no leg pain, numbness, or weakness from a compressed nerve)
- No clear surgical target — meaning the MRI doesn’t show a herniated disc or stenosis that explains the pain
- Modic type 1 or type 2 changes on MRI at one or two lumbar levels
- Failure of conservative treatments including physical therapy, medications, and injections
This procedure is not for everyone with back pain. It’s for a specific subset of patients whose pain originates from inside the vertebral body. The Modic changes on MRI are the essential diagnostic clue. Without them, the procedure doesn’t apply.

What the data shows
Basivertebral nerve ablation is supported by randomized controlled trial data showing durable pain relief. The SMART trial demonstrated statistically significant and clinically meaningful reductions in pain and disability compared to a sham (placebo) procedure — and those results held at 5-year follow-up. This is important because many pain procedures show short-term improvement that fades. The durability of the BVNA data is one of the reasons I’ve added it to my practice.
Are you ready to meet a leading Orange County Neurosurgeon?
Why this matters
I performed a basivertebral nerve ablation recently and it made me think how often vertebrogenic pain gets written off in the average spine surgeon’s office. The patient had the classic presentation — deep midline pain, worse with sitting and flexion, no radiculopathy, no clear surgical target. The kind of patient who gets labeled “nonspecific low back pain” and sent through the usual cycle without anyone asking: what if the pain is coming from inside the bone?
That bright signal on MRI inside the vertebral body isn’t just a radiological curiosity. It’s active inflammation, and the basivertebral nerve carries that signal. Once you learn to recognize the pattern, you start seeing it everywhere. A lot of patients who’ve been told they’re “non-operative” may actually have a treatable pain generator that everyone has been looking past.
Recovery
Recovery is quick. Most patients are back to normal activity within a few days. There are no activity restrictions beyond common sense in the first week. There’s no brace, no physical therapy protocol, and no device to manage. Some patients notice improvement within weeks; for others, it takes up to 3 months for the full effect as the inflammatory process in the bone settles after the nerve is ablated.

Why Choose Dr. Alexander Taghva
Dr. Alexander Taghva is a leading board-certified neurosurgeon, specializing in brain surgery, endoscopic spine surgery, as well as spine disorders. Also, he is the only spine surgeon in Orange County and southern California who offers endoscopic laminotomy surgery. Dr. Taghva:
- Graduated from John Hopkins University School of Medicine and completed his residency at the University of California
- Completed a prestigious fellowship at The Ohio State University in Neuromodulation and Functional Neurosurgery
- Specializes in minimally invasive and endoscopic surgery, spinal stenosis, artificial disc replacement, spinal disorders, spinal surgery revision, and other spinal conditions.
- Specializes in brain surgery to treat trigeminal neuralgia, brain tumors, pituitary tumors, and Parkinson’s disease.
- A highly-respected neurosurgeon with many years of experience, including treating chronic pain via stimulation of the spinal cord and brain
- Actively involved in medical research and the lead investigator for clinical trials on spinal cord stimulation




